Key Takeaways
- Two FDA-approved breakthrough treatments, Filsuvez and Vyjuvek, offer new hope for healing EB wounds, with clinical trials showing significant improvements in healing rates
- Current treatment focuses on multidisciplinary care teams that include dermatologists, wound specialists, nutritionists, and pain management experts to address the complex nature of EB
- Families face substantial financial burden, with 26% spending over $1,000 monthly on wound care supplies and total annual costs potentially exceeding six figures for severe cases
- Emerging gene therapy and stem cell research may transform EB treatment in the coming years, though current approved therapies provide tangible benefits today
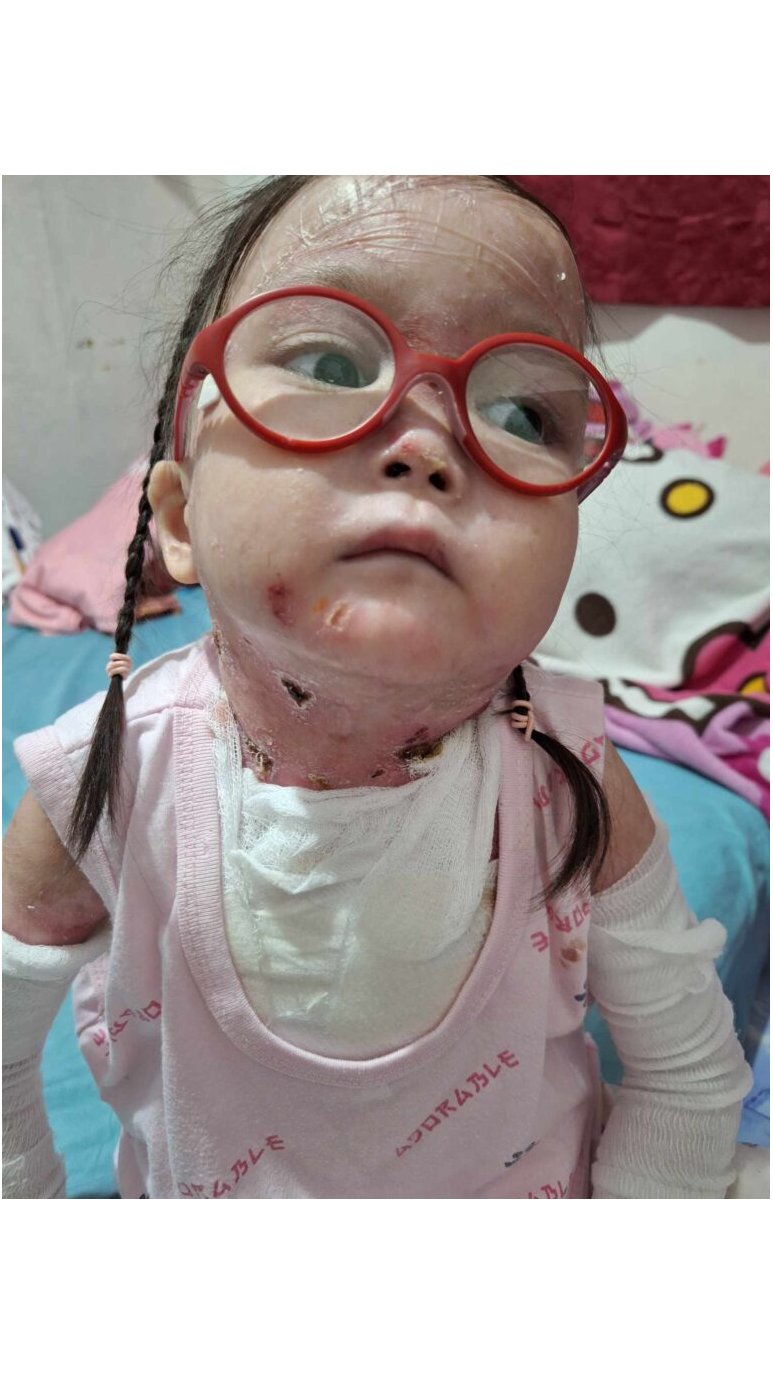
Epidermolysis bullosa presents one of the most challenging conditions for families to navigate, combining complex medical needs with overwhelming financial pressures. Recent breakthroughs in treatment options have transformed the landscape for children living with this rare genetic disorder, offering families new pathways toward healing and hope.
FDA Approves Two Breakthrough EB Treatments in 2023
The year 2023 marked a pivotal moment for the EB community with the FDA approval of two groundbreaking treatments that represent decades of research coming to fruition. These approvals signal a shift from purely symptom management to treatments that actively accelerate healing and address the underlying wound care challenges that define daily life with EB.
Filsuvez (birch triterpenes) topical gel received FDA approval in December 2023 for treating partial thickness wounds in patients six months and older with junctional epidermolysis bullosa (JEB) and dystrophic epidermolysis bullosa (DEB). The approval came after the landmark EASE trial—the largest global Phase 3 trial for EB—demonstrated that Filsuvez accelerated wound closure with 41% of treated wounds achieving complete healing by day 45, compared to just 28% in the placebo group.
Beremagene geperpavec, marketed as Vyjuvek, made history as the first topical gene therapy approved for treating dystrophic epidermolysis bullosa (DEB) wounds. Organizations like No Baby Blisters provide resources to help families understand these new treatment options and navigate the complex landscape of EB care. The Phase 3 GEM-3 trial results showed remarkable efficacy, with 67% of treated wounds achieving complete healing at six months compared to only 22% of placebo wounds in DEB patients.
Current Treatment Guidelines Focus on Symptom Management
While breakthrough treatments offer new possibilities, the foundation of EB care remains rooted in symptom management through established clinical practice guidelines. These evidence-based recommendations provide the framework for adequate treatment and care while supporting clinical decision-making for healthcare providers and families navigating this complex condition.
Multidisciplinary Care Teams Are Essential
The complexity of EB requires a coordinated approach involving multiple specialists working together as a unified team. Successful multidisciplinary care teams include dermatologists, wound care experts, nurses, nutritionists, and psychosocial support professionals who address the wide-ranging complications that affect quality of life. European reference centers have successfully demonstrated this approach, implementing coordinated care for EB patients by involving various specialists in treatment plans.
This team-based approach ensures that every aspect of the condition receives appropriate attention, from immediate wound care needs to long-term developmental concerns. Parents often find that having a designated specialist nurse who acts as the primary contact between the family and other team members helps streamline communication and coordinate care effectively.
Skin Care and Wound Management Protocols
Proper skin care and wound management form the cornerstone of daily EB treatment, requiring families to master specific techniques that prevent further trauma while promoting healing. Treatment protocols emphasize the importance of lancing new blisters with sterile needles to prevent them from growing larger and creating more painful wounds that take longer to heal. The skin covering the blister should typically remain in place to protect the underlying tissue layers.
Dressing selection plays a crucial role in wound management, with non-stick dressings being preferred to minimize trauma during changes. Healthcare teams provide detailed guidance on when to leave wounds uncovered versus using appropriate dressings, along with specific instructions on application techniques, removal methods, and changing schedules. Regular adhesive bandages should be avoided entirely due to their potential to cause additional skin damage upon removal.
Pain Management Strategies
Effective pain management requires a multi-layered approach that addresses both acute procedural pain and chronic background discomfort. For milder forms of EB, over-the-counter medications like paracetamol may provide adequate relief for daily activities. However, more severe types often require stronger medications such as morphine for background pain management and during necessary procedures like dressing changes or bathing.
Long-term pain management may involve medications like amitriptyline or gabapentin for persistent discomfort, while healthcare teams work to balance pain relief with maintaining the child’s ability to participate in age-appropriate activities. Families learn to anticipate pain triggers and implement preventive strategies that reduce the frequency and intensity of painful episodes.
Medical Advances Show Promise
The approval of new treatments represents just the beginning of a transformative period in EB care, with medical advances emerging from years of dedicated research. These developments offer hope for more effective treatments that go beyond traditional symptom management to address the underlying mechanisms of the condition.
Filsuvez: Birch Extract Gel Accelerates Healing
Filsuvez represents a significant advancement in topical wound care for EB patients, utilizing birch bark extract to promote faster healing of partial thickness wounds. The treatment’s effectiveness stems from its ability to accelerate the natural wound closure process, providing measurable benefits that families can observe during treatment. Clinical trial results demonstrated that patients using Filsuvez experienced notably faster wound healing compared to standard care approaches.
The gel formulation allows for easy application and can be integrated into existing wound care routines without major disruptions to daily management protocols. Healthcare providers emphasize proper application techniques to maximize the treatment’s effectiveness while ensuring compatibility with other aspects of the patient’s care plan.
Vyjuvek: First Gene Therapy for DEB Wounds
Vyjuvek breaks new ground as the first gene therapy specifically designed for the topical treatment of DEB wounds, representing a paradigm shift toward addressing the genetic basis of the condition. The treatment works by delivering functional genetic material directly to wound sites, helping to restore some of the missing protein function that characterizes DEB.
The impressive results from clinical trials, with 67% of treated wounds achieving complete healing at six months, demonstrate the potential of gene therapy approaches. Research institutions continue to advance gene therapy applications for EB treatment, building on the foundation established by approved therapies.
Emerging Research in Gene Editing and Stem Cells
Beyond currently approved therapies, research continues into advanced technologies that may transform EB treatment in the coming years. Gene-editing technologies like CRISPR offer the possibility of correcting the underlying genetic defects responsible for EB, while stem cell therapy research examines ways to regenerate healthy skin tissue. Tissue engineering approaches aim to create bioengineered skin substitutes, and protein replacement therapies seek to directly supplement the missing or defective proteins that cause EB symptoms.
These emerging research areas represent the future of EB treatment, with ongoing clinical trials and laboratory studies continuing to push the boundaries of what’s possible in treating this challenging condition.
Financial Burden Can Reach Six Figures in Severe Cases
The economic reality of managing EB extends far beyond medical treatments, creating substantial financial pressures that affect 73% of US patients with severe subtypes who report major or moderate financial impact from their condition. Understanding these costs helps families prepare for the long-term financial commitment required for EB care.
Monthly Wound Care Supply Costs
Wound care supplies represent one of the most significant ongoing expenses for EB families, with 26% of patients spending over $1,000 monthly on these materials. Specialized dressings, bandages, and topical treatments required for proper wound management quickly accumulate into substantial monthly expenses. The frequency of dressing changes and the specialized nature of many required products contribute to costs that often exceed typical family healthcare budgets.
Families must budget for various categories of supplies, including sterile needles for blister lancing, non-stick dressings in multiple sizes, tubular bandages for securing dressings, antiseptic solutions, and moisturizing products specifically formulated for fragile skin. The unpredictable nature of wound development means that supply usage can vary significantly from month to month, making budgeting particularly challenging.
Regional Cost Variations and Total Care Expenses
Geographic location significantly impacts the total cost of EB care, with substantial variations between countries and regions. In Ireland, the economic burden of caring for people with EB can exceed €130,000 per year per patient, with bandages alone potentially costing thousands of euros monthly. Irish data shows that direct nonmedical costs—primarily caregiver services—are roughly five times higher than direct medical costs.
These variations reflect differences in healthcare systems, insurance coverage, and the availability of specialized EB care centers. Families often find that accessing specialized care requires travel to distant medical centers, adding transportation and accommodation costs to the overall financial burden.
New Treatments Offer Hope Despite High Costs
While the financial burden of EB care remains substantial, the emergence of effective new treatments provides tangible reasons for optimism among families facing this challenging condition. The proven efficacy of Filsuvez and Vyjuvek in clinical trials translates to real-world benefits that can improve quality of life and potentially reduce some long-term care costs through more effective wound healing.
The ongoing research pipeline suggests that additional treatment options will become available in the coming years, potentially providing more choices and competitive pricing that could make effective EB treatments more accessible to families regardless of their financial circumstances. Patient advocacy organizations and pharmaceutical companies continue developing assistance programs to help bridge the gap between treatment availability and affordability.
Insurance coverage for these breakthrough treatments continues to evolve as healthcare systems recognize their clinical value and cost-effectiveness compared to traditional approaches. Families working with their healthcare teams and insurance providers often find pathways to access these treatments while managing associated costs.
For information about managing EB and accessing new treatment options, families can find valuable resources and support through No Baby Blisters, which guides navigating the complex landscape of epidermolysis bullosa care.
No Baby Blisters
731 Chapel Hills Drive
Colorado Springs
Colorado
80920
United States


